A new report into onshore detention centres cuts the improbable boasts of Scott Morrison and Peter Dutton to shreds, writes Max Chalmers.
In September 2014, 24-year-old asylum seeker Hamid Kehazaei had his life support turned off by the staff at Brisbane’s Mater Hospital. Kehazaei had been a prisoner in the Manus Island detention centre until a skin infection spread through his body and morphed into a fever that left him comatose. As the young Iranian’s health critically deteriorated on Papua New Guinea, a vital medical evacuation to Australia was delayed by the Department of Immigration.
In spite of compelling evidence to the contrary, then Immigration Minister Scott Morrison assured reporters that Kehazaei had received “outstanding” care while held in one of the further reaches of Australia’s immigration detention system, as well as after he was finally transferred onshore.
“When someone becomes ill they receive outstanding care from the people who work as part of our mainland detention network, and in the offshore processing centres that are under the management of the governments of Papua New Guinea and Nauru,” Morrison insisted.
Six months later, Morrison’s replacement Peter Dutton insisted health facilities on the tiny Pacific island of Nauru were better than some found in regional Australia and – incongruously – added that they compared favourably to field hospitals used by Australian troops fighting in Afghanistan.

If Morrison and Dutton’s assurances sounded improbable at the time, they look openly ridiculous now, in the wake of a highly critical report by the Australian National Audit Office (ANAO) examining the delivery of health services in onshore detention centre.
In fact, they look like lies.
The truth is that these Ministers, like the Department they oversee, are in no position to speak with such confidence.
That’s because, according to the ANAO’s audit, the Department of Immigration has done a poor job crafting the criteria it uses to assess the performance of private health company International Health and Medical Services (IHMS), which holds the $430 million contract for onshore health services. This appears to be the result of a warped approach that places administrative outcomes over the actual welfare of the people in detention, as well as straight-up administrative bungling.
Not only did the audit find the key measures of service delivery had been poorly designed, it also revealed that eight out of the 17 of these measures had been insufficiently implemented or not put into practice at all. One particularly important measure – supposed to assess the quality of primary health care being delivered – “was yet to be monitored 15 months after the contract was signed”.
If that sounds incomprehensibly bureaucratic then consider the impact as described in a withering section of the audit summarising the above shortcomings.
“As a consequence,” it concludes, “the department is not well placed to effectively monitor the delivery of health services.”
To put it another way, for all Morrison and Dutton’s bluster, their own Department is in no position to speak with confidence about the quality of the healthcare provided by IHMS to asylum seekers who, by the way, not infrequently end up dead in detention.
In fact, the audit presents a snapshot of a system in which the shared values of austerity and humans-as-deterrence continues to take a heavy toll on those contained within it.
Between February and early November 2015, 327 people were placed under “supportive monitoring” because of concerns about their mental health. Of that number, 239 were assessed as “high imminent risk”. 47 per cent of the time this happened, the person continued to be classified in this state for more than 72 hours.
We know self-harm and the deterioration of mental health are endemic in detention –the audit itself notes the “well-documented risks of mental health conditions arising in the detention environment”. But the true revelation from this report is that the Department has failed to monitor the situation while IHMS has failed to meet key outcomes which have been set for it.
IHMS, for instance, is supposed to provide people placed in the “high imminent risk” category with a clinical review at least once every 24-hours. But as the incredible graph below reveals, they’ve regularly failed to do that.
If IHMS had met this requirement, all the diamonds should be on or below the black diagonal line. Instead, the graph looks like this:
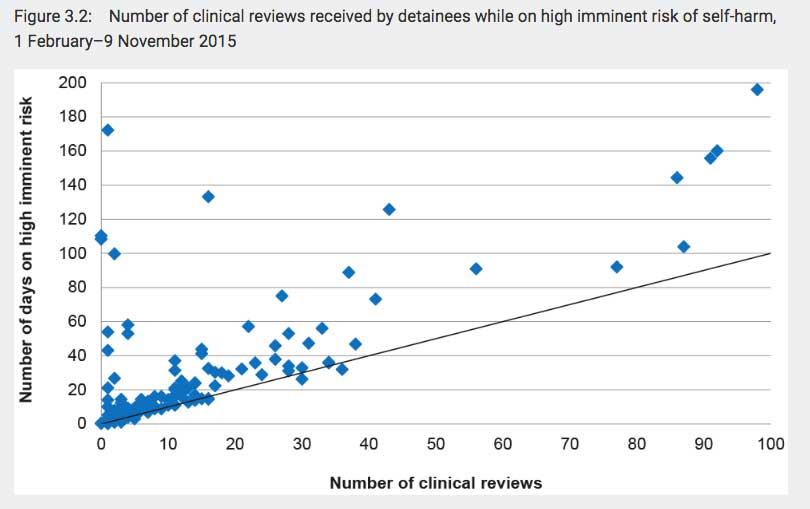
Shockingly, one person who was classified as being in a state of “high imminent risk” for around 170 days was clinically reviewed fewer than five times. They should have received this service approximately 170 times.
Given that gap between expectation and delivery, it’s hardly surprising that the audit also revealed IHMS had been docked $300,000 in the first six months of the new contract through an abatement system that offers the company rewards or deductions based on performance.
The audit found this had been the result of “a small number of significant failures” including the timeliness of its reporting as well as, more disturbingly, failures to identify and treat tuberculosis and other communicable diseases.
That’s not just a matter of filing paper work incorrectly – it’s an actual service failure that may have made people sick.
The audit also notes a set of reviews by the Department and an external consulting firm in 2015 partially verified some allegations of “alleged improper conduct” levelled against IHMS.
The bigger picture from the audit is a system in which insufficient monitoring has still managed to turn up vexing problems. And behind these problems is the shadow of austerity, an approach to government that has cast shade over welfare and health policy on both sides of the detention centre fences.
The audit reveals that in December 2013, Tony Abbott wrote to Scott Morrison expressing his hope that, after contract renewal negotiations with IHMS were complete, “the total costs and the cost per detainee would be lower in the new contract.”
On command, Morrison secured a deal with IHMS that would reduce the fee to the government by 3 per cent per annum, plus reward the company for finding other savings. The Department estimated that in total, its new model would save 30 per cent across the life of the contract.

According to the audit, the government was concerned about “over-servicing”, a process by which companies provide more service than is actually needed in order to gouge great profits. For example, you might screen refugees who don’t actually need to be screened for a disease, and then charge the taxpayer and keep some of the cash.
The government is right to be concerned about this, though it’s also to blame for the dilemma. This is the problem you face when you invite profit-making enterprises to run prison camps and jails.
But in its anxiety about not doing too much for asylum seekers, the government has evidently done too little. According to the ANAO, there had already been evidence to suggest that in the previous contract, services had been under-delivered.
“… the risk of under-servicing by the contractor— that is where the provider prioritises commercial profitability over the delivery of services of adequate quantity and quality—received less focus. This was despite issues relating to under-servicing arising under the previous contract”.
In other words, the government has geared the system in a way that, rather than delivering too much service, IHMS is incentivized to deliver not enough services, in order to protect its profits. The manifestation of this is clear in the audit, which raises concerns about the hours and availability of health staff, as well as their workloads.
This is how our detention system now operates; a tug-of-war between private profit and government austerity that leaves the people incarcerated caught in the middle, pulled from either side.
Intriguingly, albeit slightly self-servingly, IHMS appears to agree that the government has failed to institute a system that monitors the actual wellbeing of patients as a top priority.
“Rigorous compliance will only improve the quality of care if the items being monitored reflect quality of care,” Director of Operations Damien Johnston wrote in his response to the audit.

“It is the view of IHMS that current compliance reporting is predominantly focused on achieving standards relating to contractual business reporting requirements rather than standards that are necessarily a good reflection of the quality of clinical care.”
The Department does get some good marks in the audit, especially for developing its own central structure stocked with clinically trained staff. Overall, however, things look bleak. All the more so when you consider an earlier Guardian investigation into the company and the audit’s limited scope.
The ANAO’s audit was restricted to the detention centres run on the Australian mainland and Christmas Island, places you would expect to be far easier to service given their proximity to the nation’s robust health system. That means it didn’t consider the quality of service for people held in Papua New Guinea, a country beset by health challenges where life expectancy remains just 62 years, or on Nauru, where Australia had to effectively fund a new hospital. Delivering good health services to the population Australia has stranded in and around its offshore camps is a far more difficult task.
Thanks to the ANAO we may soon know just how difficult, with the office currently auditing the contracts for offshore garrison and welfare services, which is due to be completed in late 2016.
Despite the legal architecture of offshore detention slowly crumbling, and the composition of the onshore population rapidly changing, the policy of indefinitely detaining men, women and children who arrive in Australia by boat seeking asylum remains a cornerstone of both Labor and the Coalition’s platforms.
When they tell you that the people who die as a result of their incarceration received “outstanding” care, there’s no reason to believe them.
Donate To New Matilda
New Matilda is a small, independent media outlet. We survive through reader contributions, and never losing a lawsuit. If you got something from this article, giving something back helps us to continue speaking truth to power. Every little bit counts.





